Knee
 The knee is the most common site for osteoarthritis and the demand for knee surgery is on the rise; the number of knee replacement procedures predicted to more than treble by 2030.
The knee is the most common site for osteoarthritis and the demand for knee surgery is on the rise; the number of knee replacement procedures predicted to more than treble by 2030.
Knee replacement has been relatively successful in older patients, but patient satisfaction levels remain below 90% and there are challenges to address the needs of younger and more active patients.
Our research focusses on the development and testing of both earlier stage interventions for knee osteoarthritis alongside partial and total knee replacement devices.
Total knee replacement
 Wear of joint replacements remains a major factor determining their reliability and lifetime. In the knee, abnormal mechanics, wear and loosening are key factors determining longevity; with increased failure rates in younger more active patients who live longer. The pre-clinical assessment of mechanics and wear is currently undertaken experimentally by joint simulators under a limited set of conditions, which do not take into account the wide variation of clinical conditions in the patient. We are developing experimental and computational pre-clinical test methods to determine the mechanics and wear of knee and patella-femoral replacements under a wider set of surgical and patient dependent conditions.
Wear of joint replacements remains a major factor determining their reliability and lifetime. In the knee, abnormal mechanics, wear and loosening are key factors determining longevity; with increased failure rates in younger more active patients who live longer. The pre-clinical assessment of mechanics and wear is currently undertaken experimentally by joint simulators under a limited set of conditions, which do not take into account the wide variation of clinical conditions in the patient. We are developing experimental and computational pre-clinical test methods to determine the mechanics and wear of knee and patella-femoral replacements under a wider set of surgical and patient dependent conditions.
If you'd like to hear more, please contact:
Tissue sparing interventions for the cartilage
 Defects in the knee cartilage have been found in over 60% of patients undergoing knee arthroscopy; if these defects can be effectively treated early, then the progression of osteoarthritis may be delayed, reducing the need for knee replacement surgery.
Defects in the knee cartilage have been found in over 60% of patients undergoing knee arthroscopy; if these defects can be effectively treated early, then the progression of osteoarthritis may be delayed, reducing the need for knee replacement surgery.
We have developed both laboratory and computer models of the knee that we are using to examine osteochondral repair.
We are developing decellularised natural osteochondral tissue scaffolds. We use a novel processing method to gently remove cells from tissues whilst maintaining the tissue structure. This results in a natural tissue scaffold with the properties of native tissues but which does not elicit an adverse immune response upon implantation. These scaffolds will be repopulated with the patient’s own cells once implanted in the body to regenerate the damaged tissue.
For very early stage lesions, we are developing minimally invasive self-assembling peptide hydrogels which will be able to restore the biomechanical function of softened cartilage and prevent progressive lesion degeneration.
If you'd like to hear more, please contact:
Treatments for meniscus damage and degeneration
The meniscus in the knee plays a vital role in knee biomechanics, and damage to the meniscus can lead to more rapid deterioration of the cartilage and the progression of arthritis. Meniscus surgery is 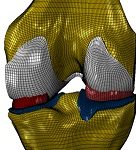 one of the most frequently performed orthopaedic procedures in the United States, but the procedures to remove or replace the meniscus tissue are not yet optimum.
one of the most frequently performed orthopaedic procedures in the United States, but the procedures to remove or replace the meniscus tissue are not yet optimum.
We have developed decellularised porcine medial meniscus scaffolds. These have been translated and used in clinical trials with Tissue Regenix PLC who are in the process of commercialising these scaffolds for routine clinical use in patients.
Additionally, we are developing decellularised meniscus-bone scaffolds which also incorporate the natural skeletal attachment sites. We are testing these in the laboratory to see whether we can improve surgical fixation and integration.
We have developed both laboratory and computer models of the knee that we are using to examine the role of the meniscus and evaluate new treatment approaches.
If you'd like to hear more, please contact:
Treatments for ligament damage
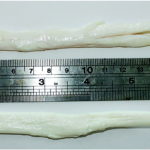 Injuries to the anterior cruciate ligament (ACL) are associated with increased risk of tears to the meniscus, the development of cartilage lesions and early onset of osteoarthritis.
Injuries to the anterior cruciate ligament (ACL) are associated with increased risk of tears to the meniscus, the development of cartilage lesions and early onset of osteoarthritis.
Novel acellular biological scaffolds are being investigated for anterior cruciate ligament reconstruction. Methods for decellularising tendons with and without bone blocks at the ends have been developed. These scaffolds have performed well in large animal studies to regenerate the ACL. The dynamic structural properties and fixation methods are now being assessed to optimise the graft properties for different populations. Tests on different sterilisation methods are also being undertaken.
